
In July 1976, the Pennsylvania chapter of the American Legion held its annual state convention at the Bellevue-Stratford Hotel in Philadelphia. About 4,000 members attended. In the days that followed the convention, 221 of the attendees became ill and 34 died from a mystery form of pneumonia. The Centers for Disease Control (CDC) immediately began investigating the disease, initially looking at viral causes. By January 1977, they had identified and isolated a bacterial source for the respiratory issues, and later named it Legionella pneumophila. These Legionella bacteria were breeding in the cooling tower of the hotel’s air conditioning system. The air circulated by the system contained small droplets of water that held the bacteria, infecting guests as they breathed in the air at the hotel.

Once the cause of the Philadelphia outbreak was determined, CDC investigators uncovered instances of the disease dating back to 1959. One of the significant outbreaks discovered was at St. Elizabeth’s Psychiatric Hospital in Washington, DC. In 1965, 81 people associated with the hospital came down with pneumonia and 14 patients at the hospital died. The infection was traced to water in a lawn sprinkler system. Specimens of the water were saved and, once Legionnaires’ disease was identified in 1977, the specimens were re-examined and matched the strain that infected the Legionnaires in Philadelphia in 1976.

Of course, the occurrence of this bacteria is not limited to the United States. The single largest outbreak of Legionnaires’ disease happened in Murcia, Spain. Between July 7 and July 22, 2001, over 800 suspected cases were reported, 449 of which were confirmed. The outbreak was linked to the cooling towers at a city hospital.
In 2003-2004, bacteria in a petrochemical plant’s cooling tower resulted in 86 cases of Legionnaires’ disease throughout the community of Pas-de-Calais, France. Various reports state that 18-21 of those who were infected died from the disease, the worst outbreak of Legionnaires’ in French history. After this incident, scientists learned that the airborne bacteria can spread much farther than originally suspected. Also, the outbreak happened in two phases: the first wave of illness happened after the cooling tower was shut down and the second happened during the cleaning of the contaminated tower and after it reopened. It’s believed that the cleaning methods used to decontaminate the tower, using high-pressure cleaning equipment, may have contributed to the second spread of the disease.
Fast forward to the summer of 2019, when guests staying at the Sheraton Atlanta Hotel between June 12 and July 15 became ill with Legionnaires’ disease. 13 people, including one who died, were diagnosed with the disease and over 60 “probable cases” were reported, the largest Legionnaires’ disease outbreak ever in the state of Georgia. Health authorities investigated and found Legionella bacteria in the hotel cooling tower, as well as in a decorative fountain in the hotel’s atrium. The hotel closed voluntarily to remove the bacteria and undergo inspections to ensure there was no Legionella risks at the hotel, reopening about a month later.

Since 2000, the number of reported cases of Legionnaire’s disease in the United States has jumped from about 1,000 to nearly 10,000 in 2018. The reported number could be well below the actual number, as the disease may be underdiagnosed. Special testing is required to determine whether a person has Legionnaire’s disease, as opposed to other strains of bacterial pneumonia, and those tests aren’t always conducted or aren’t even available in some countries. Some researchers estimate as many as 70,000 or even 100,000 people in the U.S. get the disease each year.
Similar to Legionnaires’ disease, but not as severe, Pontiac fever is a flu-like illness that’s also associated with Legionella bacteria. In 1968, workers at the county health department Pontiac, Michigan came down with flu symptoms, but not pneumonia. After the discovery of Legionnaires’ disease, blood samples from the Pontiac workers were re-examined and it was determined that their illness had been caused by the same bacteria. Victims of Pontiac fever typically recover in 1-3 days with no treatment. Because it resolves itself, Pontiac fever is never reported or goes undiagnosed, so it’s more widespread than records show.
Today, in light of building closures and slowdowns during COVID-19, the risk of Legionnaire’s disease and Pontiac fever rises. When buildings sit idle, the plumbing and HVAC systems are typically turned off to save money. This results in warm, stagnant water sitting in the systems, creating a breeding ground for bacteria. When workers come back and the systems are turned on, the bacteria can be distributed throughout the building. Even some of the buildings leased by the CDC were found to contain Legionella bacteria in their water sources after being closed for several months during the pandemic. Those buildings are undergoing remediation to ensure the bacteria is removed before workers return.
What is Legionnaires’ disease?
Legionnaires’ disease is a type of pneumonia, or lung infection, with symptoms that include cough, shortness of breath, muscle aches, headaches and fever, caused by Legionella pneumophila bacteria. Most healthy people are not affected by the bacteria, but those who are over 50 years old, current and former smokers, people with weakened immune systems and those with chronic disease are at higher risk. Most people recover when hospitalized and treated with antibiotics, but about 10% of those who get the disease die from it.
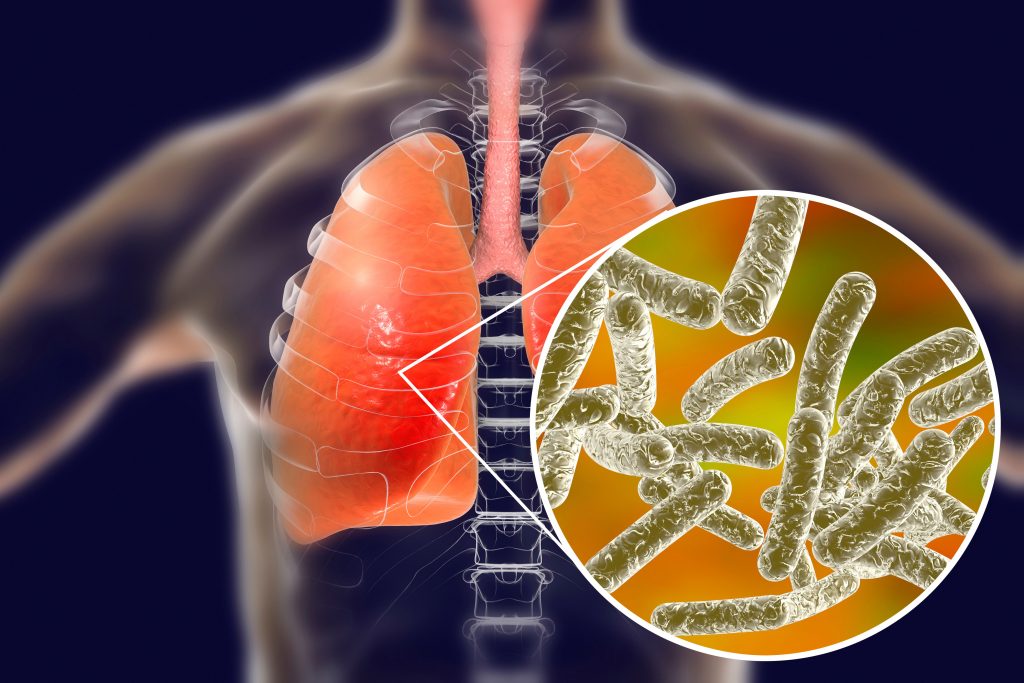
What are Legionella bacteria and how does it spread?
Legionella bacteria, or Legionella pneumophila, is the bacteria that causes Legionnaires’ disease. It grows naturally in freshwater environments, but can be found in other common water sources, including cooling towers, showerheads and sink faucets, hot, decorative fountains and water features, hot water tanks and heaters, and large plumbing systems. The cooling towers are part of industrialized air-cooling systems that are used as cost-effective HVAC systems in commercial buildings, including large office buildings, schools, hotels, hospitals and cruise ships. Cooling towers are also used to cool water that’s used in the manufacturing processes of power plants, petroleum refineries, food processing plants and other facilities. Even home humidifiers can become a breeding ground for Legionella bacteria.

The vast majority of cases of Legionnaire’s disease are contracted by breathing air that is contaminated with the bacteria. When water is used in the HVAC or cooling system, the air circulating in the building contains small droplets of water. If the water contains Legionella bacteria, it is inhaled in normal breathing. It is possible, but unlikely, to contract Legionnaires’ disease by accidentally getting water in the lungs while drinking water contaminated with Legionella pneumophila—this occurrence is very rare.
Relative humidity (RH) can help or hurt the transmission of Legionnaire’s disease. In areas with 40%-60% RH, the air’s hydration slows the travel and minimizes the reach of bacteria, which thrives on moisture. When the air carrying the bacteria is dry, the bacteria dies. When humidity levels rise above 60%, the bacteria’s survival rate improves, thereby increasing the risk of infection. The higher relative humidity generally experienced in summer months can lead to summertime outbreaks like those at the Bellevue-Stratford Hotel and Sheraton Atlanta Hotel.
How does Legionnaires’ disease compare to today’s COVID-19 coronavirus?
Both Legionnaires’ disease and COVID-19 affect the respiratory system and have the same symptoms, noted above. The primary difference in the two illnesses is that COVID-19 is viral and Legionnaires’ is bacterial. COVID-19 is highly contagious, and is most frequently spread through coughing or sneezing. Legionnaires’ disease is only contracted by breathing or aspirating the Legionella pneumophila bacteria, as detailed above. Generally, Legionnaires’ disease is not contagious, although it is possible in rare cases.
What can be done to prevent Legionnaires’ disease outbreaks?
The key to stopping Legionnaire’s disease is proper disinfection and maintenance of the water systems, HVAC systems, and humidification systems where Legionella pneumophilia bacteria thrive. Buildings that have been closed, in particular, should focus on disinfection and maintenance before workers and customers come back. Some regions have government regulations in place to help reduce the occurrence of legionella bacteria. In the United Kingdom, for example, the government’s Health and Safety Executive (HSE) suggests using a dipslide for weekly microbiological monitoring of wet cooling systems and it’s recommended that the systems should be tested for legionella bacteria at least quarterly—more frequently if the system has already had an incidence of legionella bacteria or if it’s a newly commissioned system. In Malta, new cooling towers and evaporative condensers have been prohibited in health care facilities and schools, to try to limit the potential for bacterial issues, and the country requires that cooling towers and water fountains be tested twice each year for Legionella bacteria.
One of the keys to preventing the growth of Legionella pneumophila bacteria in building systems is to limit the growth of the bacteria in potable water. Look at the size of hot water tanks and ensure that they’re properly sized. To minimize Legionella, water held in tanks should be maintained at the proper temperatures: at or below 20°C (68°F) and at or above 60°C (140°F). Inspect plumbing systems and look for places where water can stagnate, such as dead legs. Places that harbor stagnant water should be corrected to help minimize the growth of bacteria. Water in building systems also needs to be monitored and treated continually, to maintain the concentrations of free residual chlorine that minimizes bacteria growth. Usually 1-2 milligrams per liter at the tap will provide the proper level, but each system’s manufacturer’s recommendations should be followed.

Also, make a point to limit growth of Legionella pneumophila bacteria in water-cooled and heat-transfer systems. Systems should be disinfected, then maintained and operated, including treating with the appropriate biocides, in accordance with the manufacturer’s recommendations. Look at the placement of cooling towers, ensuring that they’re away from public, building make-up air. Installing drift eliminators on cooling tower can help reduce fugitive water droplets that may host bacteria.
Being mindful of the places where bacteria are likely to grow in building systems is the first start to preventing outbreaks. Check with governmental agencies who have jurisdiction over the area to ensure you’re following any mandatory service and inspection guidelines and consult with the manufacturer of your cooling tower manufacturers for information specific to your system. Industrial trade organizations are often a good resource for guidance in avoiding the spread of Legionella pneumophilia, too. If it’s not something you want to manage on your own, there are specialized companies dedicated to water system management that focus solely on Legionella pneumophila, who can be contracted for ongoing control services.
As businesses continue to open after being shut down or having their operations slowed by COVID, the risk of Legionella pneumophila affecting facilities is higher. By properly inspecting, disinfecting and managing building systems, you can minimize the occurrence of this dangerous bacteria and reduce the risk of Legionnaire’s disease, Pontiac fever and other illnesses that can result from these harmful water-borne bacteria.
For a downloadable PDF of this article, click HERE.

